Orbital Fracture: Symptoms, Treatment & Recovery
A clear guide to symptoms, evaluation, and healing after an eye socket fracture.
Overview
An orbital fracture is a break in one or more of the bones that form the eye socket (the orbit). Because some orbital walls are very thin, fractures can happen even from a moderate impact—sports injuries, falls, or accidents.
Not every fracture is the same. Some are small and stable, while others change the shape of the orbit or restrict the tissues that help the eye move. That’s why a fracture can be “present” on a scan but not require surgery—or, in other cases, require timely repair to protect function and symmetry.
If you want a broader view of trauma evaluation and reconstruction, see Eye Trauma.
At a Glance
- Typical symptoms: swelling, bruising, double vision
- Common concern: restricted movement or eye position change
- Imaging: CT scan is commonly used
- May need surgery if: entrapment, persistent diplopia, large defects
- Recovery: bruising/swelling often improve in ~2 weeks
- Goal: comfortable single vision + natural eye position
What an orbital fracture actually affects
The orbit isn’t just bone—it’s a “housing” for muscles, fat, nerves, and the eyeball itself. A fracture can:
- Change orbital support (risking a sunken eye)
- Create a gap where soft tissue can shift
- Restrict eye movement if tissue is tethered or trapped
- Irritate nerves, leading to numbness in the cheek or upper lip
Understanding which of these is present is what turns imaging into a practical treatment plan.
Common symptoms patients notice
- Double vision (diplopia), often worse looking up or to the side
- Swelling and bruising around the eyelids
- Pain or discomfort with eye movement
- Numbness in the cheek/upper lip (infraorbital nerve irritation)
- Change in eye position (enophthalmos) or new asymmetry
Some symptoms come from swelling and improve quickly. Others—especially persistent diplopia in everyday gaze—can signal a mechanical problem that won’t resolve without targeted treatment.
When to seek urgent evaluation
Seek urgent in-person assessment if you have sudden vision changes, severe escalating pain, inability to move the eye normally, significant nausea/vomiting with attempted eye movement (possible entrapment), or concern for a deeper injury.
Even without emergency signs, ongoing double vision, worsening asymmetry, or a clear change in eye position is a reason to schedule a specialist exam.
How diagnosis works (what the exam is looking for)
A trauma-focused exam typically includes vision testing, pupil evaluation, corneal assessment, and measurement of eye alignment and motility. The pattern of limitation matters: swelling can reduce movement “a little,” while entrapment can create a specific restriction pattern.
CT imaging is commonly used to define the fracture, estimate defect size, and evaluate whether soft tissue appears tethered. Imaging + symptoms + measurements = treatment decision.
Treatment options: observation vs surgical repair
Observation may be appropriate for small, stable fractures with improving symptoms, no significant restriction, and minimal risk of late enophthalmos. Follow-up is still important to monitor eye position as swelling resolves.
Surgery is considered when imaging and symptoms suggest entrapment, when diplopia persists in functional gaze, when there is significant displacement, or when a large defect raises concern for late sunken-eye changes. The goal is to restore normal anatomy and support the orbital wall so the eye can sit and move naturally.
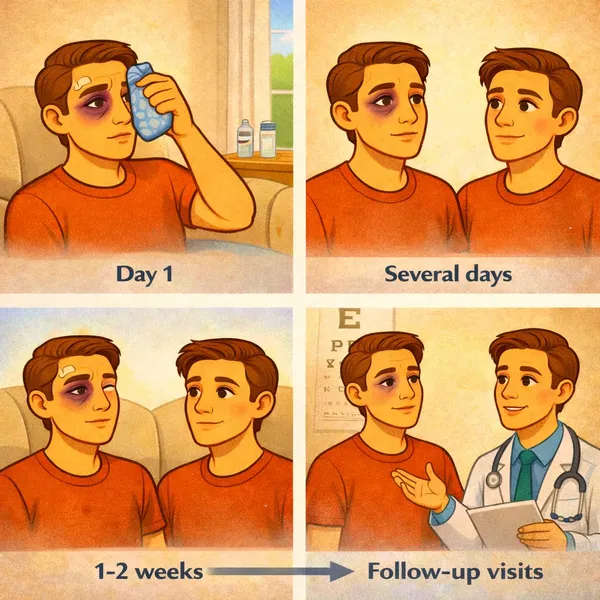
Recovery timeline: what patients usually experience
Most bruising and swelling improves noticeably within 1–2 weeks, but subtle contour refinements can continue for several weeks. Your surgeon monitors eye alignment, comfort, eyelid position, and symmetry at follow-up visits.
Patients often ask, “When will I feel normal?” Many feel significantly better after the early swelling resolves, while visual alignment improvements can be gradual depending on the cause of diplopia and the treatment plan.
Questions to bring to your consult
- Is my double vision expected to improve as swelling resolves?
- Do CT findings suggest entrapment or a large defect?
- Am I at risk for late enophthalmos (sunken eye)?
- What restrictions should I follow and for how long?
- What follow-up schedule do you recommend to track alignment and symmetry?
Having these questions ready helps you leave with a clear plan rather than uncertainty.
What orbital fracture repair aims to fix
When repair is recommended, the focus is functional and structural:
- Freeing or protecting restricted tissues
- Restoring orbital volume and wall support
- Helping the eye return to a natural position
- Reducing the risk of persistent diplopia or late asymmetry
Repair plans are individualized based on symptoms, CT findings, and exam measurements.
Practical recovery tips that matter
- Swelling control: follow your surgeon’s instructions for cold compresses and positioning.
- Activity: avoid heavy lifting and contact sports until cleared.
- Follow-up: keep appointments to track alignment and symmetry.
- New symptoms: report sudden vision changes or rapidly worsening pain.
Good recovery is rarely just “time.” It’s time + the right checkpoints.

Frequently Asked Questions
Do all orbital fractures need surgery?
No. Many fractures heal with observation when symptoms improve and imaging does not show significant entrapment or displacement. The decision is based on function, measurements, and CT findings.
How long does double vision last after an orbital fracture?
It varies. Some cases improve quickly as swelling resolves. Persistent diplopia—especially in straight-ahead or reading gaze—should be evaluated for treatable causes.
Can a fracture cause a sunken eye later?
Yes. Larger defects can change orbital volume and lead to late enophthalmos. Early specialist assessment helps identify who is at risk.
Is bruising a sign of a severe fracture?
Not necessarily. Bruising can be dramatic even with smaller injuries. The exam and CT findings are more important than bruising alone.
What if my symptoms feel worse a few days later?
Swelling can peak after the first day or two. However, sudden vision changes, severe pain, or rapidly worsening symptoms should be evaluated urgently.
Why See an Oculoplastic Surgeon?
Trauma care often needs a balance of function (vision, comfort, eyelid closure, tear drainage) and appearance (symmetry, natural contour). An oculoplastic surgeon is specifically trained for eyelid, tear duct, and orbital reconstruction.
Alexander Rabinovich, MD provides oculoplastic trauma evaluation and reconstruction in New York City and Brooklyn. If you’re experiencing double vision, restriction, or eye position changes after injury, an oculoplastic evaluation can clarify whether observation is safe or repair is advisable.
Educational content only; not a substitute for medical advice. If you have sudden vision changes, severe pain, or worsening symptoms after an injury, seek urgent in-person care.
Book an Orbital Trauma Evaluation
For an overview of services and what we treat, visit Eye Trauma. You can also book a consultation below.



Leave a reply